CME for Cardiologists: Dual Antiplatelet Therapy After Stent Placement
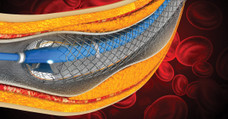
Dual antiplatelet therapy (DAPT) is the cornerstone of post-percutaneous coronary intervention (PCI) management. By combining a P2Y12 receptor inhibitor and aspirin, cardiologists can reduce the risk of stent thrombosis (ST) and other major adverse cardiovascular events (MACE) such as myocardial infarction and stroke.
The current therapeutic landscape is moving away from the 12-month, one-size-fits-all DAPT duration to provide more personalized strategies that balance the risk of ischemia with the risk of bleeding. In this guide, we’ll explore current guidelines, risk-stratification tools, and tips for choosing the right agent for your patient and procedure.
Current Guideline Overview (ACC/AHA/ESC)
Guidelines from the ACC, AHA and ESC provide duration recommendations for DAPT tailored to the patient’s condition and risk profile. Standard therapy for patients with Acute Coronary Syndrome (ACS) consists of 12 months of DAPT with aspirin and a P2Y12 inhibitor such as ticagrelor or prasugrel. If there is a high risk of bleeding, therapy may be shortened to three to six months. Patients with Stable Ischemic Heart Disease (SIHD) generally receive a shorter therapy duration, with six months of aspirin and clopidogrel and even briefer durations for those with a high bleeding risk.
While guidelines generally follow the default 12-month timeline, interventional cardiology is shifting toward shorter DAPT durations followed by P2Y12 monotherapy. Modern drug-eluting stents have much lower rates of thrombosis, making shorter DAPT durations of one to three months effective for most patients. Creating a personalized, de-escalated regimen also helps reduce bleeding risks by replacing high-intensity P2Y inhibitors, such as ticagrelor or prasugrel, with less-intense agents like clopidogrel.
Risk Stratification Tools
Assessing a patient’s DAPT score can help create a custom therapy protocol that best aligns with their risk profile. The score is calculated based on variables such as age, condition, smoking habits and stent size to determine the benefit-to-risk ratio of continuing DAPT beyond 12 months:
- A score greater than or equal to 2 indicates a lower risk of bleeding and a high risk for ischemic events, suggesting extended DAPT to lower ischemic risk.
- A score lower than 2 suggests a higher risk of bleeding and a lower risk of ischemic events, making shorter DAPT the best choice to prevent complications.
Clinicians can also examine a patient’s PRECISE-DAPT score for more information on their specific bleeding risks and recommended DAPT duration. If DAPT and PRECISE-DAPT scores conflict, the patient’s overall ischemic and bleeding risks, comorbidities and procedural factors should guide clinical decision-making.
Choosing the Right Agent
The right agent for DAPTual Antiplatelet Therapy depends on a patient’s clinical presentation, bleeding and ischemic risk and comorbidities:
- Clopidogrel is a less potent option that’s best used in patients with stable CAD who are at a higher bleeding risk, or for elderly patients with a history of stroke.
- Ticagrelor is preferred in ACS cases for its potent, reversible properties and reduced risk of ischemic events.
- Prasugrel is often reserved for ACS patients undergoing PCI who don’t have a high bleeding risk.
While not currently standard practice, genomic testing for CYP2C19 can identify clopidogrel resistance to provide genotype-guided therapy recommendations. Patients with loss-of-function alleles often have a reduced response to clopidogrel and are better suited for ticagrelor or prasugrel to ensure better protection against ischemic events.
Perioperative Management of DAPT
Balancing a patient’s stent thrombosis risk with bleeding risks guides perioperative DAPT management to minimize potential complications. If a stent patient requires non-cardiac surgery, procedures should be delayed at least six weeks for bare-metal stents and six to 12 months for drug-eluting stents. Performing surgery too soon can result in premature cessation of DAPT and lead to fatal stent thrombosis.
If a patient requires urgent surgery within three months of PCI, bridging intravenous agents may be necessary to maintain platelet inhibition. For on-cardiac surgeries with high bleeding risks, stopping the P2Y12 inhibitor for five to seven days before the operation and resuming as soon as possible helps to balance bleeding control while minimizing thrombosis risk.
The Move Toward Personalized Medicine in DAPT
Modern guidelines are moving away from a one-size-fits-all approach toward personalized DAPT based on a patient’s age, clinical condition and bleeding risk. Using risk stratification tools, interventional and general cardiologists can tailor the duration, antiplatelet agents and perioperative decisions of their treatment to create safer, more effective treatments for their patients.
For more information on interventional and general cardiology, explore Oakstone’s CME activities today. With specialty-specific filtering, you can easily find CME tailored to your interests and professional requirements.